If you ask Linda Bender about the care she received at Ellis Fischel Cancer Center, she would say it was top notch. In December, Bender and her husband traveled to Columbia from Forsyth, Missouri, to have her bladder and surrounding cancerous tissue removed in a procedure known as a radical cystectomy.
“I had a wonderful surgeon, and all of the nurses and the team were great,” she says. “I couldn’t ask for a better doctor. They explained my care to me, but when you’re in that state — it’s a tough and scary time — a lot of what they tell you goes in one ear and out the other. There’s so much to take in.”
At Ellis Fischel Cancer Center, care is centered on the needs of the patient. That’s why the hospital’s leaders have developed new enhanced recovery protocols to ensure patients have the resources they need to guide them before surgery, after surgery and once they’re discharged from the hospital.
“Surgery is more than just an experience in the hospital,” says Kevin Staveley-O’Carroll, MD, PhD, former director of Ellis Fischel Cancer Center. “It’s an entire journey, and there is a lot for patients to take in. It can be frustrating to patients if one member of their team gives them one set of instructions, but another member of the team gives differing instructions. That doesn’t help anyone. Our newly developed enhanced protocols are standardized and streamlined for optimal care.”
A patient-centered approach
Ellis Fischel leaders developed the TIGER protocols, an acronym coined by Eric Kimchi, MD, former medical director of Ellis Fischel, which stands for Team InteGrated Enhanced Recovery. The team created the protocols to enhance recovery measures after surgical procedures. Feedback from patients such as Bender helped the team at Ellis Fischel customize its approach to meet unique patient populations.
Enhanced recovery is a multidisciplinary, evidence-based approach that improves surgical outcomes through:
- Minimally invasive surgical techniques
- Goal-directed fluid therapy
- Use of short-acting intravenous anesthetics
- Minimizing the use of opioids for pain management
- Limiting routine use of tubes and drains
- Encouraging early return to normal nutrition and physical activities
“When experts from all these areas come together, the result is an overall better experience for the patient.”
- Katie Murray, DO
“Essentially, the TIGER protocols are a patient-centered approach to minimize the symptoms, enhance recovery, improve outcomes and enable the delivery of safe, effective and value-based care,” says Staveley-O’Carroll, who also serves as chair of the MU School of Medicine’s Hugh E. Stephenson Jr., MD, Department of Surgery. “They ensure that each member of the entire surgical team is on the same page and communicates a consistent message to our patients. Repetition is very important, especially during stressful times, and it’s crucial that patients and their caretakers have resources that guide them in their recovery.”
In order for patients to get the best care possible, comprehensive teams work cohesively from departments such as anesthesiology, nursing and surgery. Although Staveley-O’Carroll points to those three areas as drivers of the protocols, it requires a much larger team made up of pharmacists, dietitians, respiratory therapists, physical therapists, operating room staff, social workers, information technology specialists and more.
“When experts from all these areas come together, the result is an overall better experience for the patient,” says Katie Murray, DO, a former urologic surgeon at Ellis Fischel Cancer Center who has worked with TIGER protocol patients. “These enhanced recovery protocols
allow the patient to feel more engaged and empowered in the care they receive. Often times, this can lead to shorter hospital stays.”
Improving collaboration
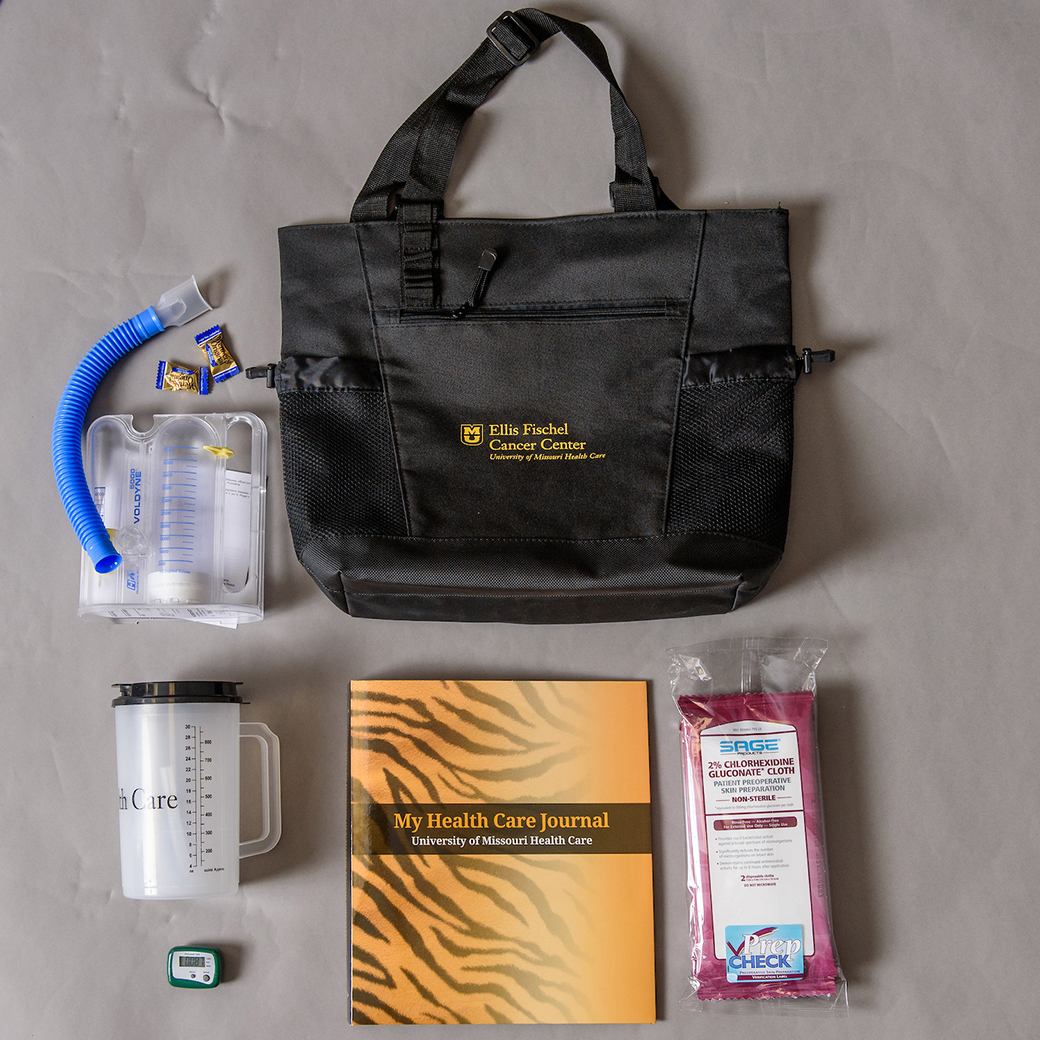
When patients are scheduled for a surgery, they are provided with a bag filled with resources and materials to help guide them on their journey toward recovery (see “TIGER Tote”). The protocols are currently established for patients undergoing radical cystectomy surgery, but plans are in place to expand the protocols for liver, pancreas, thoracic and colorectal surgeries and eventually to all surgical procedures offered at Ellis Fischel and the Department of Surgery.
“There’s been enormous success at similar organizations that have implemented their own enhanced protocols,” Staveley-O’Carroll says. “Patients experience much better outcomes, quality is improved and costs are decreased. Improving our collaboration as an entire surgical team means patients can have shorter lengths of stay in the hospital and have a reduced likelihood of being readmitted. It’s an opportunity to improve everything involved in the surgical journey. It’s a global approach that we will be applying systemwide as a cohesive team.”