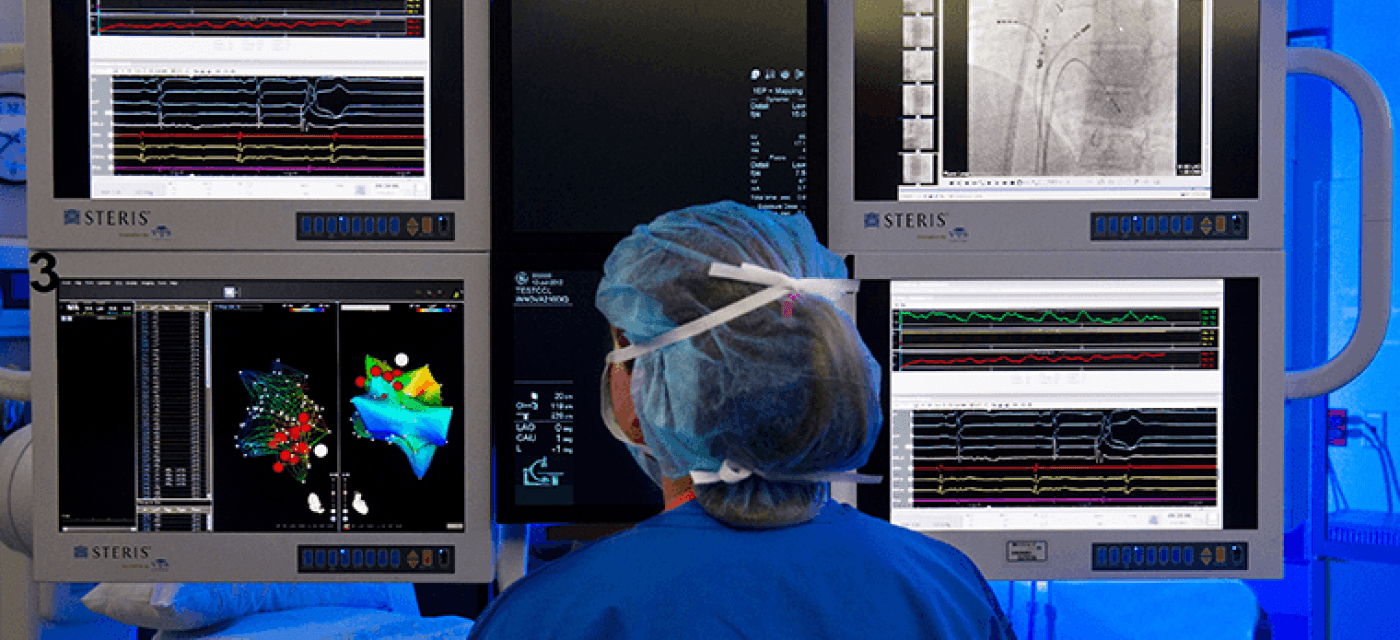
At MU Health Care, we believe a healthier heart supports a fuller, more active life. Our heart and vascular experts offer the most complete care in mid-Missouri, from prevention and diagnosis to advanced treatment and recovery.
Heart and Vascular Care at MU Health Care
We combine leading-edge diagnostics and treatments with coordinated, personalized support.
If you experience symptoms such as chest pain, dizziness or shortness of breath, our team can use advanced diagnostic tools to find the cause and create a treatment plan for your exact needs. Our specialists evaluate and treat many types of heart and vascular conditions, including:
We explain your options clearly and outline potential treatments — from medications and nonsurgical therapies to surgical procedures. Together, we can develop a plan so you can decide what aligns best with your needs and goals.
A Team Approach to Heart Health
Our team of experts from different fields works together to meet your needs and address your concerns. Your care team may include:
How Our Specialists Work Together
Our specialists collaborate together, so each step of your care is coordinated and informed by the right expertise. For example, an electrophysiologist manages heart rhythm care, an imaging doctor provides detailed scans to guide treatment options, and a pharmacist helps fine-tune medications. We will discuss recommendations with you and explain your options so you can decide how to move forward with your care.