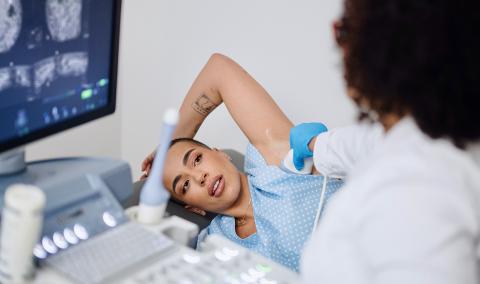
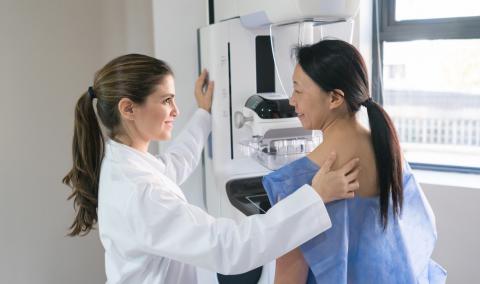
At MU Health Care, you’ll find expert breast cancer care that combines the latest research with a personal approach. Whether you’re newly diagnosed or seeking a second opinion, our team is here to support you with clarity, confidence and trusted expertise every step of the way.
We treat breast cancer with a team-based model that’s designed around you. Whether you’re being cared for at Ellis Fischel Cancer Center in Columbia or Goldschmidt Cancer Center in Jefferson City, our dedicated breast cancer teams collaborate throughout your journey, from early evaluation to survivorship, ensuring a thorough and personalized approach to your care.
Breast Cancer Symptoms
Breast cancer can develop without obvious signs, especially in its early stages. That’s why staying up to date on routine cancer screenings is so important. When symptoms do appear, they may include:
- A new lump in the breast or underarm
- Thickening or swelling in part of the breast
- Irritation, dimpling or puckering of breast skin
- Nipple discharge (including blood)
- Change in size, shape or appearance of the breast or nipple
- Pain in any area of the breast
If you notice any of these changes, schedule a breast exam as soon as possible.
Breast Cancer Risks
Women who might be at a higher risk of developing breast cancer include those who:
- Have a family history of breast cancer, particularly in a first-degree relative (mother, sister, or daughter), especially if diagnosed before age 50, or a family history of ovarian cancer at any age
- Are older, as your risk of developing breast cancer increases with age
- Have certain inherited gene mutations, such as BRCA1, BRCA2, or other genes linked to hereditary cancer syndromes
- Have certain reproductive or hormonal factors, such as early menstruation (before age 12), late menopause (after age 55), having no children or having a first child after age 30, or using hormone replacement therapy
- Are of Ashkenazi Jewish descent, which is associated with a higher likelihood of BRCA mutations
- Engage in certain lifestyle behaviors, including alcohol use, lack of physical activity, or obesity after menopause
Breast Cancer in Men
Breast cancer doesn’t just affect women. Although less than 1% of all breast cancers occur in men, it’s important to have a care team that understands the unique needs of male patients. At MU Health Care, our team provides personalized care for men who are diagnosed with breast cancer. Risk factors include:
- A family history of breast cancer
- Inherited gene mutations
- Klinefelter syndrome
- Radiation exposure
- Estrogen-related drug treatments
- Liver disease
Types of Breast Cancer
Breast cancer can take several forms. Some are fast-growing and aggressive, while others are slow to develop. Common types include:
- Ductal carcinoma in situ (DCIS): A noninvasive form confined to the milk ducts
- Invasive ductal carcinoma (IDC): The most common type, starting in the ducts and spreading into surrounding breast tissue
- Invasive lobular carcinoma (ILC): Begins in the milk-producing glands (lobules) and can spread
- Triple-negative breast cancer: A more aggressive subtype that doesn’t respond to hormone therapy
- HER2-positive breast cancer: Driven by excess HER2 protein and often responds well to targeted therapy
- Inflammatory breast cancer: A rare, fast-growing form that causes redness and swelling
Our specialists use advanced imaging and pathology to determine your exact type and guide your treatment plan.
Our Approach to a Breast Cancer Diagnosis
When breast cancer is suspected or detected on a mammogram, our team acts quickly to confirm your diagnosis and provide next steps. You’ll have access to:
- Same-day or expedited diagnostic imaging, including 3D mammography, ultrasound and MRI
- In-office, image-guided biopsies to minimize delays
- Genetic counseling and testing when needed
- Breast health nurse navigators to coordinate your appointments and care plan
From the beginning, your care team includes fellowship-trained breast radiologists, surgeons, oncologists and reconstructive specialists who meet regularly to review your case and tailor your treatment.
Breast Cancer Treatment at MU Health Care
Your treatment plan depends on your cancer type, stage and personal goals. We offer a full range of options — from standard therapies to the latest innovations — right here in mid-Missouri.
Breast Surgery
Our breast surgeons specialize in breast-conserving surgery (lumpectomy), mastectomy and lymph node procedures. We also offer immediate or delayed breast reconstruction.
Radiation Therapy
Our radiation oncologists use advanced techniques to precisely target tumors while protecting healthy tissue.
Chemotherapy
Delivered before or after surgery, chemotherapy helps destroy cancer cells throughout the body. We tailor each regimen based on your cancer’s biology.
Hormone Therapy
For hormone receptor-positive cancers, medications can block estrogen or lower hormone levels to reduce recurrence.
Targeted Therapy
Targeted therapies are available for breast cancer that is HER2 positive, which means the cancer cells have proteins that promote cancer growth, or if the cancer is hormone-receptor-positive. These two types of breast cancer can be treated through specific targeted therapies.
Immunotherapy
In some cases, especially with triple-negative breast cancer, immunotherapy may be used to help your immune system fight the cancer.
Why Choose MU Health Care for Breast Cancer Care
Dedicated Breast Cancer Teams
At both Ellis Fischel Cancer Center and Goldschmidt Cancer Center, you’ll be cared for by specialists who focus exclusively on breast cancer. Our team includes fellowship-trained experts who collaborate to develop personalized treatment plans designed for the best possible outcomes.
Faster, More Accurate Diagnoses
Our team approach and access to advanced diagnostics — like 3D mammograms and breast MRI — help us move quickly from suspicion to a precise diagnosis and treatment.
Fully Coordinated Support Services
From surgery to survivorship, our patients benefit from a fully coordinated care experience. Supportive services like cancer rehabilitation, nutrition services and counseling are offered at both Ellis Fischel Cancer Center and Goldschmidt Cancer Center, so you can access the care you need without delays or outside referrals.
Access to the Latest Research and Clinical Trials
Our breast cancer experts stay at the forefront of new treatments through research and clinical trials. When eligible, you may have access to promising therapies not widely available elsewhere in the region.
Recognized Excellence in Cancer Care
Ellis Fischel Cancer Center is Missouri’s only state-designated cancer center. Both Ellis Fischel Cancer Center and Goldschmidt Cancer Center hold national accreditations that reflect our commitment to quality, safety and continuous improvement in cancer care.